Trick or treat? The role of uric acid and central obesity on the risk of metabolic syndrome

Metabolic syndrome is a collection of conditions that happen together, increasing your risk of heart disease, stroke and type 2 diabetes. These conditions include increased blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol or triglyceride levels.
Metabolic syndrome predicts not only the risk of developing diabetes, cardiovascular diseases and chronic kidney disease, but also that of many degenerative diseases in later life.
Although both cross‐sectional and longitudinal studies have implicated abdominal obesity as the central feature of this complex condition, the pathogenesis of MetS is very complex in terms of the underlying mechanism, the sequence of development, and the interactions among individual components and with other metabolic disorders.
It is generally accepted that central obesity is a core component of metabolic syndrome (MetS). On the other hand, hyperuricemia, the predecessor of gout, has been found to cluster with multiple components of MetS. But it is unclear whether hyperuricemia is a downstream result of central obesity/MetS or may play an upstream role in MetS development.
Elevated serum uric acid (SUA) has been associated with increased blood pressure, body mass index and triglyceride, and reduced HDL-C. Hyperuricemia also predicts the development of MetS, insulin resistance, hypertension and diabetes.
Nonetheless, so far, hyperuricemia has not been included as a component of the syndrome MetS. A comprehensive map of such a complex syndrome will help to create strategies for prevention and management.
To address this question, we carried out a Mendelian randomization study using genomic data of 10,000 participants from Taiwan Biobank (TWB). The aim of the TWB is to establish a population-based database, gathering information from 200,000 volunteers on genetic, lifestyle and environmental factors.
Recently, our group has discovered that the peak age of onset for hyperuricemia occurs earlier than that of hypertension and diabetes in a Taiwanese cohort study. Based on this, they hypothesized that uric acid may have a causal relationship with the components of MetS.
In this regard, a Mendelian randomization (MR) study was conducted by analyzing data from a total of 10,000 participants of the Taiwan Biobank. MR technique exploits the random distribution of genetic variants at the gametogenesis phase, enabling their use as instrumental variables for testing the causality and is less likely to be affected by confounding or reverse causation than conventional observational studies.
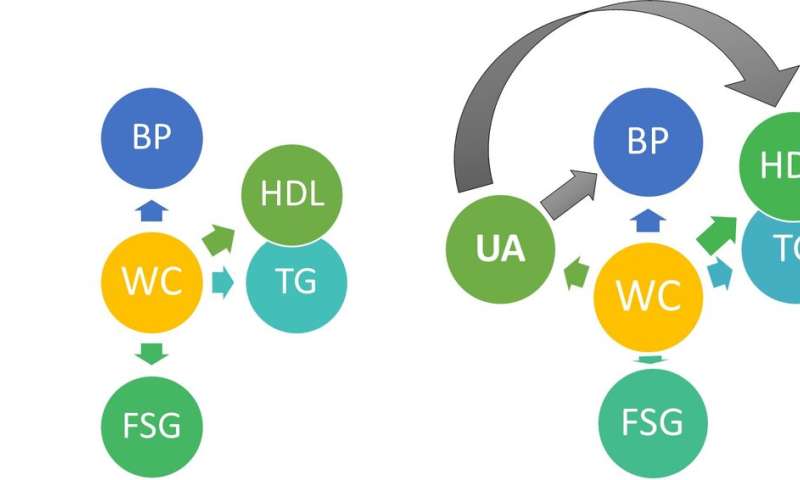
Our investigation shows that uric acid increment may augment the risk of MetS through increasing blood pressure and triglyceride levels and lowering HDL-C values, but not through accumulating fat or hyperglycemia. High waist circumference may be a causal agent for all the components of MetS, including hyperuricemia. Moreover, our previous MR study results support the idea that hyperuricemia may play a causal role in cardiovascular disease development.
In other words, our study shows that genetic predisposition to higher levels of uric acid is causally associated with blood pressure elevation and dyslipidemia components of MetS, but not obesity/diabetes components, suggesting that SUA may involve a separate pathway of MetS development independent of obesity.
Findings like these may alter clinical thinking such that uric acid control can be prioritized to the same extent as obesity, dyslipidemia and hypertension. Whether hyperuricemia may be considered as a therapeutic target for preventing MetS warrants further studies. The findings from this study have been published in the International Journal of Obesity.
This story is part of Science X Dialog, where researchers can report findings from their published research articles. Visit this page for information about ScienceX Dialog and how to participate.