Cancer vaccines revitalized by antigenic essence technology
Recently, cancer vaccine development has been complemented by our antigenic essence technology. Considering that the creation of cancer vaccines is a constant priority for research and biotechnology, the emergence of new technology in this field is a significant event, especially because previous technologies have not yielded results. In this article we introduce readers to antigenic essence technology, omitting some technical aspects and allowing certain liberties in the interpretation of scientific facts in favor of a reader-friendly narrative.
Cancer and evolution
Cancer is a major health problem worldwide and the second leading cause of death in the United States. What makes this disease so dangerous? The famous biologist Theodosius Dobzhansky said, "Nothing in biology makes sense except in the light of evolution." The nature of cancer can therefore be described in terms of evolutionary theory. Species develop as a result of mutations and selection affecting organisms; by analogy, cancer cells develop by mutation and selection among cells, under pressure from the body's defense mechanisms. Thus, the development of cancer is a reflection of the evolutionary process at a cellular level.
The connection of cancer with the force that provides variety to life, including human existence, explains why cancer is so pervasive; it can come to anyone at any time and in different forms. The evolutionary nature of cancer development is underlined by the fact that it is both difficult to cure and tends to relapse—the drivers of evolution are not flimsy. This means that the fight against cancer sometimes requires brutal means, with serious consequences for health. Chemotherapy, in fact, entails poisoning the body in the hope that the cancer cells will die faster than the patient. It is a very difficult course of treatment that many patients refuse even though refusal means certain death.
Cancer and vaccines
Since cancers are diverse and often arise suddenly, treatment must be both specific and flexible, and ideally long-lasting. It is obvious to us that vaccination offers all of these benefits. One or just a few injections of a vaccine can lead to long-term protection of the body by activating the body's natural defenses.
So why don't we have a cancer vaccine yet? The answer is pretty simple. Cancer cells are just altered cells of our own body. Humans possess around 20,000 genes, each of which could be mutated in many ways. Melanoma, a particularly aggressive form of skin cancer, expresses at most 150 mutations. Lung and colorectal cancers have similar numbers of mutations, and other cancers have even fewer. From these and other data we know that the molecular composition of a cancer cell is very close to that of a normal cell. Therefore, the principle of vaccination that works against bacteria and viruses (vaccinate with what you want to develop protection against) does not work against human cancer cells because the result would be the body attacking itself. One possible solution lies in the use of neoantigens—antigens expressed from mutated genes only. Unfortunately, 99% of the mutations in cancer are not critical to the cancer's survival, so targeting them wouldn't necessarily kill the cancer.
In our opinion, similar limitations can also be found in vaccinations that use separate cancer antigens, including chimeric antigen receptor technology and mRNA vaccines. It is theoretically possible to destroy a pool of cancer cells by triggering the immune system with one or several antigens. However, since most cancers are heterogeneous, cells that express the targeted antigens to a lesser extent will survive and continue to mutate. The high mutation rate of cancer cells gives them a major evolutionary advantage over slower-mutating healthy cells. To expect that the selection pressure of a vaccine caused by one or only a few antigens will radically change the fate of cancer is highly doubtful and has not yet been realized in practice.
Background for new technology
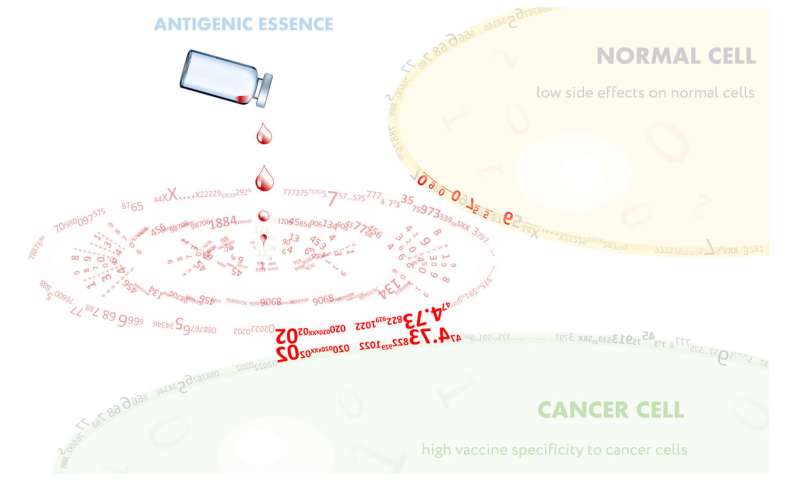
Autoimmune diseases are characterized by a body's immune system attacking its own healthy cells. In order to prevent such a situation arising from a cancer vaccine, it will be necessary to induce a very selective immune response. That is, the immune system must be able to clearly distinguish between cancer cells and healthy cells, so that it only targets the cancer. Just as we humans recognize one another by looking at each others' faces, immune cells recognize target cells by looking at the molecules on their surfaces.
Thus, we thought it would not be very smart to vaccinate with whole cancer cells, since 99% of the cell is inside the cell and ignored by the immune system anyway. Antibodies and killer cells sent by the immune system recognize only antigens presented on the surface of cancer cells, because they do not penetrate inside. Moreover, many of the molecules found within the cell are concerned with basic cellular functions such as biosynthesis, energy balance, and cell division, and are common to all cells of the body. It has become clear to us that attempts at conventional vaccination using whole cancer cells have tended to generate side effects and autoimmune reactions, rather than targeting cancer cells, due to the existence of this nonspecific content. In contrast, the surface of a cell is where its individuality is expressed. A multitude of environmental factors, including contacts with nearby cells, contacts with the surrounding structures, and the presence of various receptors, contribute to the unique "face" of each cell type.
Antigenic essence technology
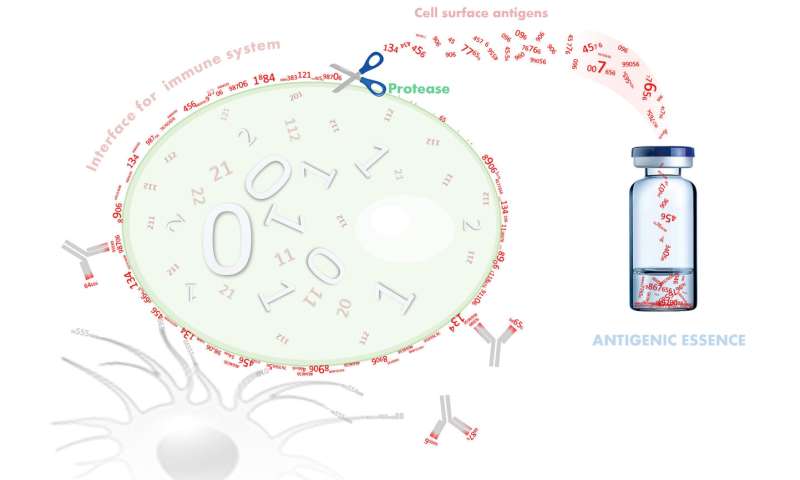
So it dawned on us that for effective cancer vaccination, we need to collect the "face" of the cancer cell. The bulk of specific molecules in a cell are proteins. In order to split proteins from the cell surface, it is simply necessary to treat the living cells with a protease—an enzyme that cleaves proteins. Since the protease is rather large, it does not penetrate inside the cell and therefore only cleaves the proteins available on the surface.
However, there are numerous proteases. How to choose the right one? Not only must we collect the cell's "face" as completely as possible, we must also avoid destroying it. We found that the protease trypsin fully cleaves surface proteins while also maintaining their cell specificity. The cellular "face" collected in this way was called antigenic essence which, like a key to a lock, precisely fits the cancer cells from which it was collected. When, in the experiment, almost all cancer cells were killed by the antigenic essence, we were disappointed, believing that the experiment had failed for some reason, because this seemed impossible. But, just in case, we processed the data we obtained and we were stunned—the results fit the model, indicating the effectiveness of the antigenic essence. This discovery is radically changing our understanding of anticancer vaccination. We now believe that antigenic essence is the ideal composition for cancer vaccination.
Doubts
Adherents of outdated vaccination approaches may justifiably doubt that it could be so simple. Splitting the surface off of a cancer cell to get a natural, highly targeted product that is free from the bulk of nonspecific substances seems pretty obvious. Why haven't scientists already tried this approach? Again and again, decade after decade, people have tried to create vaccines based on inactivated cancer cells; despite repeated failure in clinical trials, this approach is still being used! In defense of scientists, we can say that vaccines based on antigenic essences could not have appeared earlier. For all their apparent simplicity, they require the cutting-edge science of proteomics: the large-scale study of proteins. The technological aspects of obtaining an antigenic essence is summarized in detail in our article "Antigenic essence: upgrade of cellular cancer vaccines" published in Cancers.
Final remark
Of course, hope always remains, and even if antigenic essence fails it will not be the end of cancer vaccines. The highest evolutionary achievement of homo sapiens is his mind, and this mind will always come up with something to give us new hope. But today we hope that thanks to antigenic essence, we already have something to believe in.
This story is part of Science X Dialog, where researchers can report findings from their published research articles. Visit this page for information about ScienceX Dialog and how to participate.
More information: Petr G. Lokhov et al. Antigenic Essence: Upgrade of Cellular Cancer Vaccines, Cancers (2021). DOI: 10.3390/cancers13040774
Bio:
Dr. Petr Lokhov, born in 1973, a citizen of the Russian Federation, married, has two children. Dr. Lokhov has been working at the Institute of Biomedical Chemistry (Moscow) since 1995. In 1995, he held the position of laboratory assistant. In 1996, he received a diploma of higher education (Russian National Research Medical University, Moscow) and got the position of junior scientist. In 2010, he was transferred to the position of lead scientist, and from 2012 to the present, he is the head of the laboratory (Mass spectrometry-based metabolomic diagnostics) – the first metabolomics laboratory in Russia. Since 2001 – Ph.D.; since 2016 – Doctor of Sciences; since 2017 – expert of the RAS responsible for post-genomic technologies; since 2019 – co-founder, CEO and Chief Scientific Officer of BioBohemia Inc. (pre-clinical stage company focused on the cancer vaccine development, Delaware, USA); general scientific experience – 25 years; the author of 70 scientific papers; H-index – 15 (Scopus). Lokhov is a member of AACR, the Metabolomics Society, and HUPO. Currently, Lokhov is a leading scientist in Russia in the field of metabolomics and cancer vaccine development.